 Although this movement helps compensate somewhat for the drop in ECF osmolarity, it cannot do so completely, and the result is a decrease in ECF osmolarity and a loss of ECF volume. Because ECF osmolarity drops compared to that of the ICF, water moves from the ECF into the ICF, and thus concentrates the ECF. Individuals with Chronic Adrenocortical Insufficiency excrete a urine that is more concentrated than the ECF, causing relatively more solute loss than water from the ECF and thus a drop in ECF osmolarity.Chronic Adrenocortical Insufficiency: Hypoosmotic Contraction.Although this movement helps compensate somewhat for the increased ECF osmolarity, it cannot do so completely, and the result is an increase in ECF osmolarity and a loss of ECF volume. Because ECF osmolarity rises compared to that of the ICF, water moves from the ICF to the ECF. Individuals with Diabetes Insipidus excrete a urine that is more dilute than the ECF, causing relatively more loss of water than solutes from the ECF and thus a rise in ECF osmolarity. 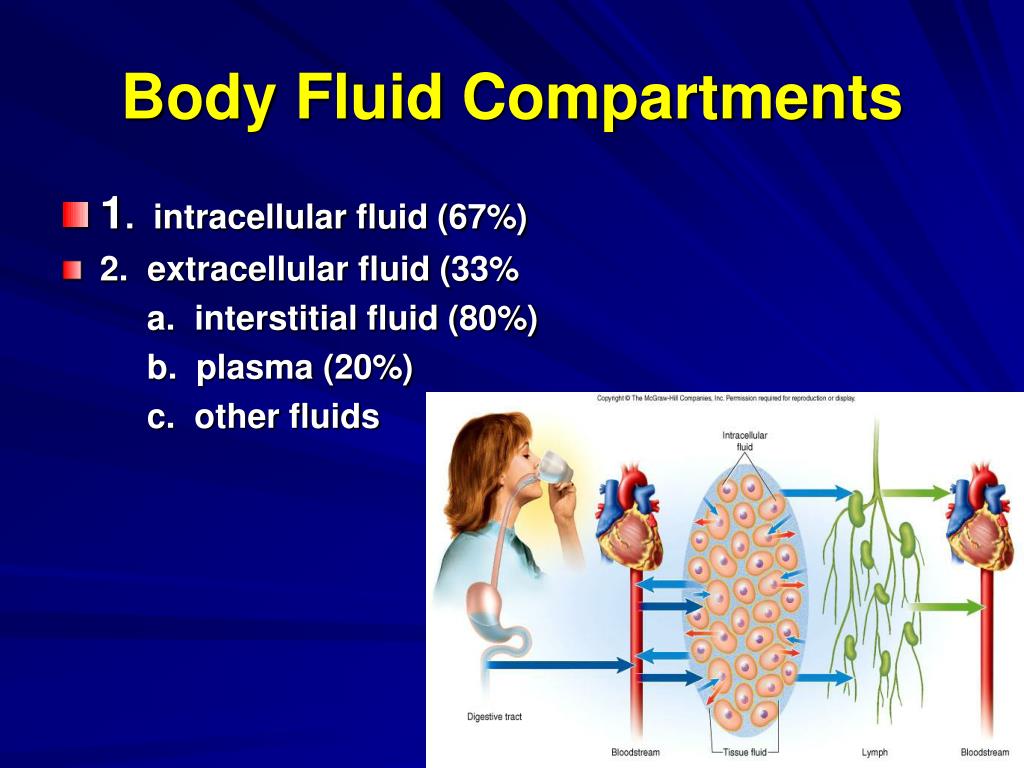
Diabetes Insipidus: Hyperosmotic Contraction. 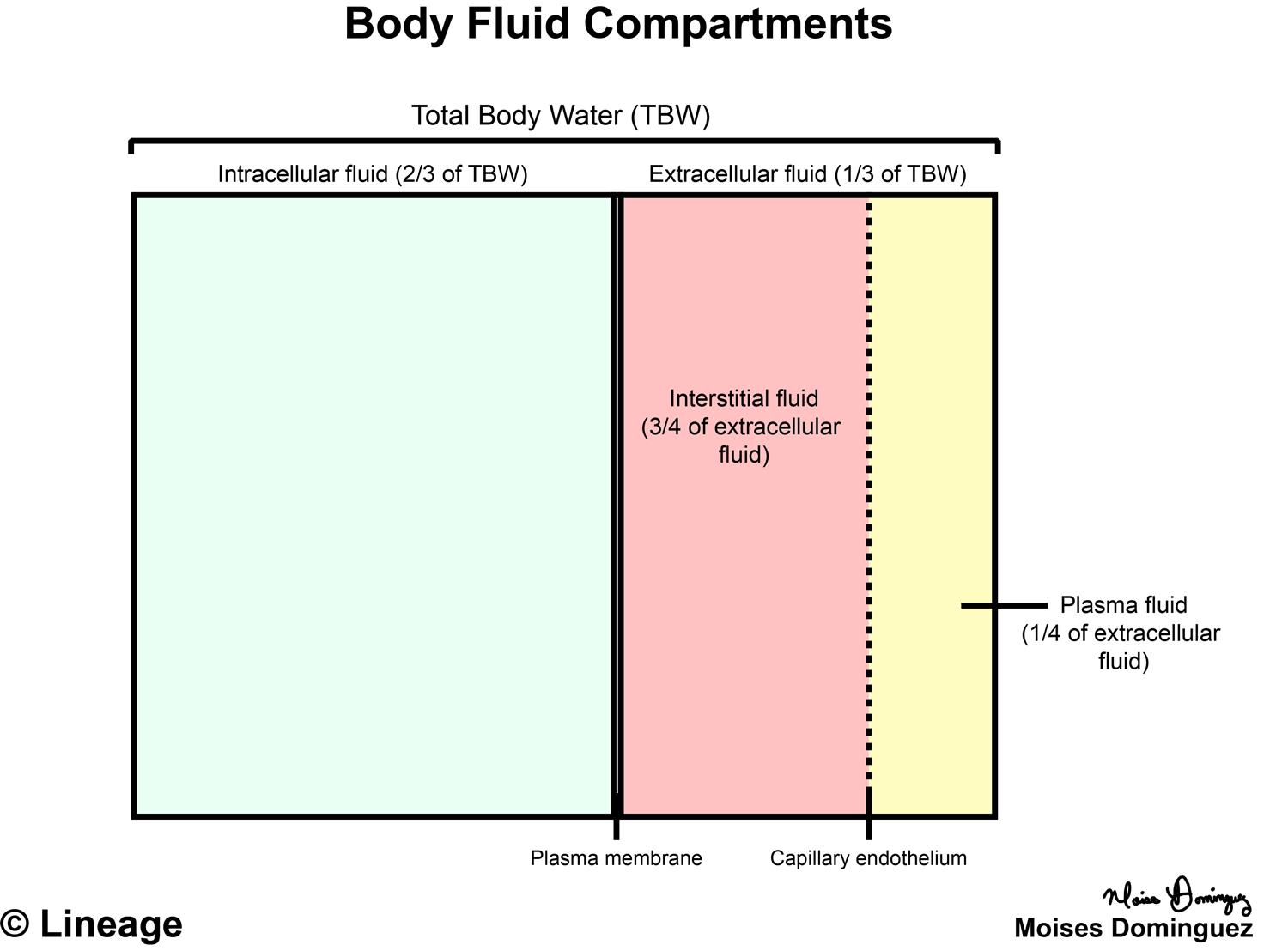
As a result, there is no shift in body fluid between the ICF and the ECF and thus the total volume of the ECF contracts due to its loss within in the diarrheal fluid. 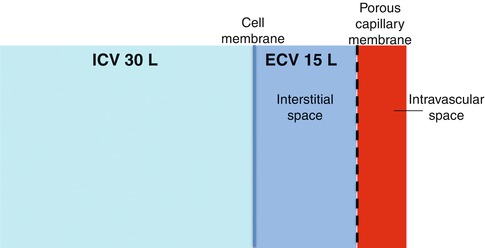
In cases of secretory diarrhea, fluid is secreted from the GI tract with precisely the same osmolarity as that of the ECF consequently, there is no change in the ECF osmolarity.Secretory Diarrhea: Isoosmotic Contraction.Note, that the below examples are relatively simplified and do not take into account complex homeostatic mechanisms which are brought into play, especially by the kidneys during contexts of fresh water intake. Any shifts in fluid volume between compartments purely follows from the change in ECF osmolarity. The key step when evaluating these disturbances is to identify what effect the disturbance has on the ECF osmolarity. With the above basic principles in mind, it is relatively easy to predict how fluid volume will shift in the body during a variety of pathological scenarios.These figure are not to scale and thus the reader should not try to interpret the quantitative values of the osmolarity and volume, but should focus on their qualitative increase or decrease. In the case of secretory diarrhea, no change in ECF osmolarity is caused and thus there is no shift in fluid between the ICF and ECF. As seen, the driving force for the shifting fluid is a change in the ECF's osmolarity. The initial change from normal is given above followed by the compensatory body fluid shift below. the volume (x-axis) of the body's ICF and ECF during states of pathological volume loss. 
These graphs provide a representation of the osmolarity (y-axis) vs. Once the ECF osmolarity changes, water shifts into or out of the intracellular compartment, within minutes, until a new osmolar equilibrium is achieved between the ECF and ICF. Solutes and water can be added to it from the GI tract whereas they can be subtracted from it by a variety of processes, most notably by the action of the kidneys but also by loss from perspiration, breathing, and the feces.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
